NewsLetter
February 2026 | Volume 8 | Issue 1
* Click on Topic to Read

A Milestone Year for SNHPE: Building Bridges among Health Professionals
1,2Raju Srivastava
1Professional Development Director, Society of Nepalese Healthcare Professionals in Europe (SNHPE)
2Expert in Medical Radiation Physics, Universitair Ziekenhuis Gent, Belgium.
The Society of Nepalese Healthcare Professionals in Europe (SNHPE) was established in August 2024 with the mission of fostering professional collaboration, academic exchange, and career development among Nepalese healthcare professionals across Europe. The Society aims to facilitate or organize networking events; deliver educational and professional development programs; and support initiatives that strengthen the healthcare sector in Nepal through strategic partnerships and collaborative projects.
Uniting clinicians, nurses, public health experts, biomedical scientists, researchers, allied-health practitioners, and students, SNHPE operates as a non-profit, non-political, and professionally driven organization. It is committed to supporting Nepali healthcare professionals throughout the European Union and the European Economic Area (EEA/EFTA), while contributing to the enhancement of Nepal’s healthcare system. The SNHPE serves as a dynamic platform for multidisciplinary collaboration and continuous professional development. The Society regularly hosts webinars and academic events featuring experts from both Europe and Nepal, promoting the exchange of clinical knowledge, scientific innovation, and health-system best practices. Through mentorship initiatives and networking opportunities, it provides structured support for early-career professionals and students as they advance through their educational and professional pathways.
On 9–10 August 2025, the Society successfully held its First Ordinary General Assembly in Amsterdam, The Netherlands. The assembly was inaugurated by H.E. Ms. Sewa Lamsal, Ambassador of Nepal to BENELUX and the EU. Thirty-six participants from various European countries attended the assembly, which featured clinical, scientific, and IT sessions, along with literary and musical programs.
Attendees also enjoyed a traditional Nepali dinner accompanied by musical performances by the executive board members and others. During the assembly, Prof. Dr. Ganesh Acharya, MD, PhD, FRCOG from Sweden, was honored with the Nepalese Healthcare Professional of the Year 2025 Award in recognition of his outstanding contributions to medicine.

In his address, Prof. Acharya reflected on his journey from rural Nepal to becoming a leading figure at one of the world’s top university hospitals. The award will be presented annually to Nepalese health professionals in Europe who have demonstrated exceptional contributions in medicine, nursing, or health-science research.

As part of its commitment to celebrating excellence in healthcare, the Society has also introduced the Europe Nepal Health Award. This award recognizes individuals, groups, or institutions that have made significant contributions to improving healthcare delivery in Nepal or advancing the professional rights of Nepali health workers. The award includes a certificate and a monetary prize of NPR 100,001. SNHPE has selected the Nepal Medical Association (NMA) as the inaugural recipient, acknowledging its dedicated efforts, advocacy, and achievements in securing improved rights and allowances for resident doctors in Nepal in 2025.
Looking ahead, SNHPE is delighted to announce the launch of the European Journal of Nepalese Healthcare Professionals (EJNHP) – a biannual, online, open-access journal aimed at providing a rigorous, peer-reviewed platform for high-quality research, case reports, and scholarly work relevant to clinical practice, public health, and healthcare systems. The first issue is scheduled for publication in May–June 2026. The journal welcomes submissions of original research, review articles, case reports, and academic contributions from healthcare professionals and researchers across disciplines and regions, with a commitment to nurturing a vibrant and diverse academic community.
The Society of Nepalese Healthcare Professionals in Europe looks forward to continued coordination, cooperation, and collaboration in advancing its mission. The Society warmly welcomes eligible Nepalese healthcare professionals across Europe to join its membership and contribute to its shared goals.

Beyond the Algorithm: The Multidisciplinary Role of AI Researchers in Medical Physics
Md Saib Hossain
United International University, Bangladesh.
Introduction: We are currently witnessing a paradigm shift in healthcare often described as the “Golden Age” of Artificial Intelligence (AI). For decades, medical physics has relied on computational modeling to understand radiation interactions and imaging mechanics. However, the role of the AI researcher in this field has evolved from simple automation to becoming a critical partner in clinical decision-making. Today, AI researchers are not merely writing code; they are solving the “last mile” problems in radiation oncology and diagnostic imaging, translating complex deep learning theories into life-saving clinical tools.
Contribution of Human Element: A multidisciplinary approach to successful AI implementation is never the work of a single profession; it requires a robust ecosystem of human resources. The “AI Researcher” acts as the architect, designing models (such as U-Nets or GANs) that can interpret complex medical data. However, this work is impossible without a multidisciplinary team:
- Medical Physicists: They act as the bridge between code and clinic, performing rigorous Quality Assurance (QA) to ensure the AI’s output is physically possible and safe for patient use.
- Radiation Oncologists & Radiologists: These specialists provide the “Ground Truth” the expert-labeled data required to train algorithms. Without their high-quality inputs, even the most advanced model will fail (“Garbage In, Garbage Out”).
- Radiation Therapists (RTTs): As the frontline users, they validate whether an AI tool (like auto-contouring) actually saves time in a real-world workflow or merely adds complexity.
- IT & PACS Specialists: They ensure the seamless flow of data between the AI server and the hospital’s image database, a critical often-overlooked role.
Transforming Radiation Therapy: The most immediate contribution of AI researchers lies in radiation therapy planning. Historically, contouring Organs at Risk (OAR) and tumor targets was a labor-intensive manual process. Recent advancements in Deep Learning, specifically convolutional neural networks (CNNs), have enabled the automation of this task with sub-millimeter accuracy. Current research in 2025 is moving beyond simple segmentation. AI researchers are now developing generative models, such as Generative Adversarial Networks (GANs), to create “synthetic CT” scans from MRI data. This innovation allows patients to receive radiation plans based on MRI soft-tissue contrast without requiring the additional radiation dose of a planning CT scan. Furthermore, Reinforcement Learning (RL) agents are being deployed to optimize dose distribution, effectively “playing” the treatment planning game to maximize tumor control while sparing healthy tissue.
Revolutionizing Diagnostic Imaging: In diagnostic physics, the focus has shifted toward image reconstruction and quality assurance (QA). AI researchers are developing algorithms that can reconstruct high-fidelity images from sparse data, enabling faster MRI scans and lower-dose CT protocols without compromising diagnostic quality.
A critical area of contribution is “predictive maintenance.” By analyzing the vast streams of log data from linacs and scanners, AI models can now predict equipment failures before they occur, ensuring that treatment schedules remain uninterrupted. This shift from reactive to proactive QA is a direct result of collaboration between computer scientists and clinical physicists.
The Generative Frontier: The newest frontier for AI researchers is Generative AI and Large Language Models (LLMs). Beyond pixels, these models are now being adapted to handle multimodal data combining images, patient history, and genomic data into a single diagnostic reasoning engine. Researchers are exploring how these models can draft medical notes, summarize complex patient histories for tumor boards, and even simulate patient physiology as “Digital Twins” to test treatment outcomes virtually before physical application.
Conclusion: The integration of AI into medical physics is no longer a futuristic concept; it is a clinical reality. However, this power comes with responsibility. The primary role of the AI researcher today is to ensure these systems are safe, explainable, and equitable. By collaborating closely with medical physicists, AI researchers can ensure that the algorithms of tomorrow do not just process data, but truly care for patients.
References
1. Collective Minds. (2024, October 27). AI in medical imaging: Key research advances 2025. https://collectiveminds.health/articles/medical-imaging-research-breakthroughs-in-ai-and-advanced-technologies
2. International Atomic Energy Agency. (2024). Artificial intelligence in medical physics: Roles, responsibilities, education and training. https://www-pub.iaea.org/MTCD/Publications/PDF/TCS83web.pdf
3. Iori, F., Cappelli, A., D’Angelo, E., Cozzi, S., Ghersi, S. F., De Felice, F., Ciammella, P., Bruni, A., & Iotti, C. (2025). Photon GRID radiation therapy: A physics and dosimetry white paper. New Approaches in Radiotherapy, 17(12), 1980. https://doi.org/10.3390/cancers17121980
4. Open MedScience. (2025). Computational modelling and AI in medical physics: Transforming healthcare through innovation. https://openmedscience.com/computational-modelling-and-ai-in-medical-physics-transforming-healthcare-through-innovation/
5. Signify Research. (2025, January 6). Generative AI in healthcare: 2024’s breakthroughs and what’s next for 2025. https://www.signifyresearch.net/insights/generative-ai-news-round-up-december-2024/
6. Smith, J., & Doe, A. (2025). Generative AI in clinical (2020–2025): A mini-review of applications. Journal of Medical AI, 12(3), 45–52. https://pmc.ncbi.nlm.nih.gov/articles/PMC12620437/
7. Avanzo, M. (2025). Why medical physicists in artificial intelligence? SCMPCR Newsletter. https://scmpcr.org/wp-content/uploads/2025/02/1.-Why-medical-physicists-in-artificial-intelligence_Michele-Avanzo_Final.pdf

Synergy of Care: Inside the Radiotherapy Ecosystem
Meher Nigar Sharmin
Khwaja Yunus Ali Medical College and Hospital, Enayetpur, Sirajganj, Bangladesh
Exploring the Seven Pillars of Radiotherapy Excellence
Radiotherapy represents far more than advanced machinery or clinical protocols; it is a dynamic and deeply human enterprise built on expertise, empathy, and coordinated effort. Each patient’s experience unfolds through the commitment of professionals who bridge the divide between science and compassion, ensuring that every beam of radiation is guided not only by precision but also by care. In this write-up, we highlight seven foundational roles within the radiotherapy landscape, individuals whose collaboration transforms complex technology into meaningful treatment. From the oncologist’s strategic clinical oversight to the physicist’s meticulous dosimetric calculations, from the technologist’s calming presence to the nurse’s attentive vigilance, each professional contributes uniquely to a shared mission: to treat, to support, and ultimately, to restore.
- Radiation Oncologist — Architect of the Therapeutic Path:
Central to the delivery of radiotherapy is the radiation oncologist, whose role extends beyond prescription to encompass the conceptualization and orchestration of individualized treatment strategies. Informed by a robust understanding of tumor histopathology, radiobiological response, and patient-specific variables, the radiation oncologist delineates treatment objectives—curative, palliative, or disease-stabilizing with precision. Treatment planning is conducted in accordance with internationally endorsed guidelines, including those from ESTRO, ASTRO, and the ICRU, ensuring adherence to best practices and consistency across clinical settings. Through multidisciplinary collaboration with medical physicists and radiation technologists, the oncologist ensures that therapeutic plans are both dosimetrically rigorous and contextually appropriate. From simulation to follow-up, their clinical stewardship integrates technical accuracy with an ongoing commitment to patient-centered care.
- Medical Physicist — The Mind of Precision, The Engineer Behind Every Beam:
If the radiation oncologist determines the therapeutic objective, the medical physicist defines how that objective is realized—with rigor, safety, and scientific precision. Every treatment plan originates from their quantitative analyses, and every radiation beam depends on their meticulous calibrations. Employing advanced modalities such as 3D conformal radiotherapy (3DCRT), intensity‑modulated radiotherapy (IMRT), volumetric‑modulated arc therapy (VMAT), image‑guided radiotherapy (IGRT), simultaneous integrated boost (SIB), craniospinal irradiation (CSI), stereotactic radiosurgery (SRS), and stereotactic radiotherapy (SRT or SBRT), medical physicists sculpt radiation delivery to align with individual anatomical and dosimetric parameters. Their work is continuously benchmarked against international quality assurance frameworks, including those established by the International Atomic Energy Agency (IAEA) and the American Association of Physicists in Medicine (AAPM). Through systematic verification and daily quality control, they translate complex physical principles into consistent, reliable clinical practice quietly ensuring that technology remains a trustworthy extension of therapeutic intent.
- Radiation Therapy Technologist (RTT) — Precision Meets Presence
Often serving as the most familiar presence throughout the treatment course, the Radiation Therapist (RTT) translates complex planning into precise clinical execution. Operating sophisticated linear accelerators, RTTs ensure sub-millimetric patient alignment and verify positioning through real-time imaging and adaptive protocols. Their technical proficiency is indispensable to maintaining treatment accuracy and reproducibility. Yet, beyond the realm of precision and process, RTTs embody the human continuity of radiotherapy. They provide reassurance in moments of uncertainty, foster trust within the clinical environment, and transform technologically intensive procedures into experiences grounded in empathy and care. Each treatment session unfolds under their steady guidance, reflecting a seamless integration of technical mastery and patient-centered compassion.
- Radiotherapy Nurse — The Human Touch in High-Tech Care
From initial consultation through to post-treatment follow-up, the radiotherapy nurse constitutes a continuous and stabilizing presence within the care continuum. Their responsibilities encompass the proactive management of treatment-related toxicities, ongoing monitoring of physiological parameters, and the facilitation of communication between patients and the multidisciplinary care team. Beyond clinical duties, they play a pivotal role in patient education, psychosocial support, and advocacy—ensuring that individuals are not only medically safeguarded but also emotionally sustained throughout the radiotherapy process. In many respects, the radiotherapy nurse functions as the integrative thread that binds the technical, clinical, and human dimensions of oncologic care.
- Patient Attendant — Foundational Support in the Therapeutic Encounter
Long before the initiation of radiation delivery, a more immediate and often understated form of care takes place. Patient attendants serve as the first point of contact within the radiotherapy environment, facilitating physical transfers, providing orientation within clinical spaces, and guiding patients through unfamiliar procedural norms. Their presence, marked by consistency and attentiveness, restores a sense of dignity through small but deeply human interactions. Though their role may unfold largely in the background, the psychological and emotional reassurance they provide constitutes an essential component of the patient experience.
- Biomedical Engineer — Custodian of Technological Integrity
The precision of radiotherapy is fundamentally dependent on the reliability of its technological infrastructure. Biomedical engineers occupy a critical yet often invisible role in maintaining this integrity. Their responsibilities encompass the calibration, maintenance, and operational troubleshooting of key systems such as linear accelerators, imaging simulators, and ancillary equipment. Through proactive vigilance and adherence to safety protocols, biomedical engineers sustain treatment continuity and uphold technical accuracy—both of which are foundational to therapeutic efficacy.
- Industry Vendor — Strategic Partner in Clinical Advancement
Vendors in the radiotherapy domain extend far beyond the function of equipment provision. They serve as long-term collaborators, facilitating the integration of novel technologies, offering training and technical support, and ensuring the clinical team remains abreast of system updates and innovations. By maintaining a responsive interface between manufacturers and medical institutions, vendors contribute to operational sustainability while upholding ethical and regulatory standards. Their engagement is instrumental in enabling departments to evolve in step with the pace of scientific and technological progress.
Together, They Form the Radiotherapy Care Ecosystem
While each role within the radiotherapy continuum carries its own domain of expertise, none operates in isolation. It is through interdependence—clinical, technical, and emotional—that a fully integrated care ecosystem emerges. Within this framework, precision is inseparable from compassion, and innovation is aligned with patient-centered values. Radiotherapy, then, is not merely the delivery of treatment; it becomes an orchestrated process of healing—sustained by trust, collaboration, and shared purpose.

Becoming a GREMP Mentee: Reflections on Learning, Mentorship and Building Research Skills in AI-Driven Medical Physics
Mohammad Ullah Shemanto
Evercare Hospital Chattogram, Bangladesh
Medical physics in low- and middle-income countries (LMICs) is dominated by heavy clinical workloads, leaving limited opportunity for research, despite rapidly expanding radiotherapy services. In Bangladesh, medical physicists are responsible for treatment planning, machine commissioning, quality assurance, imaging QA, and radiation safety, often with little protected time or mentorship for research. As a result, local contributions to advanced medical physics research, especially in artificial intelligence (AI), remain limited.
My selection as a mentee in the Global Research and Mentorship Program (GREMP) marked a major shift in my professional journey from a clinically focused physicist to an emerging researcher in AI-driven cancer outcome modeling. This article summarizes my GREMP experience, from proposal development to mentorship, interdisciplinary collaboration, and skill building.
GREMP: A Global Research Capacity-Building Model
GREMP was established to strengthen medical physics and cancer research capacity in LMICs by pairing early-career professionals with experienced international mentors. Unlike short-term fellowships, GREMP is a longitudinal, mentorship-driven program focused on developing sustainable research skills such as problem formulation, study design, data analysis, and scientific writing.
Selection into GREMP is competitive and based on motivation, scientific potential, and commitment rather than prior research output. I was selected as a GREMP mentee and, to my knowledge, the only medical physicist from Bangladesh in this program. This carried both professional significance and responsibility to represent my country and build local research capacity.
A key figure in this process was Dr. Manju Sharma, PhD (UCSF), Chair of the GREMP subcommittee. She provided strategic guidance during proposal development, ensured appropriate mentor matching, and supported access to validation datasets, helping ensure scientific rigor and sustainability of the project.
Mentorship Structure and Proposal Development
GREMP follows a three-member mentorship model: one global mentor, one local mentor, and one mentee.
My mentors were:
Mentorship Structure and Proposal Development
Global Mentor: Dr. Sharon Qi, PhD, DABR (Associate Professor, UCLA)
Local Mentor: Prof. Dr. Hasin Anupama Azhari (United International University; Director, South Asia Centre for Medical Physics and Cancer Research)
My initial proposal broadly focused on head-and-neck cancer. Under Prof. Azhari’s guidance, this was transformed into a scientifically structured research plan with defined hypotheses, endpoints, and methodology. I then presented the proposal before a GREMP evaluation panel and was selected based on scientific merit, motivation, and readiness to learn.
From Clinical Thinking to Site-Specific AI Modeling
Once paired with Dr. Sharon Qi, my research perspective changed fundamentally. Drawing on her expertise in outcome modeling and imaging-guided radiotherapy, she emphasized that biological and site specificity are critical for AI. Head-and-neck cancer is highly heterogeneous, which can degrade model learning. Under her guidance, the project was refined to focus on oropharyngeal squamous cell carcinoma (OPSCC), improving biological consistency, feature learning, and model interpretability.

Learning to Work with Public Datasets
Our hospital’s limited OPSCC data could have been a barrier, but Dr. Qi reframed this as a learning opportunity. I was introduced to The Cancer Imaging Archive (TCIA) and trained in dataset selection, annotation standards, and ethical research use. I learned that high-quality AI research depends more on study design, curation, and validation than on local data volume alone.
Radiomics and Deep Learning
The project began with handcrafted radiomics, using tools such as 3D Slicer, where I learned how segmentation quality, voxel normalization, and preprocessing affect feature stability. This built my understanding of shape, first-order, and texture features. The study then progressed to deep learning–based feature extraction using convolutional neural networks on CT images. Comparing handcrafted and deep features highlighted key trade-offs between interpretability, generalizability, and predictive power in clinical AI models.
Interdisciplinary Collaboration and Skill Building
A major early challenge was my limited programming background. Prof. Azhari facilitated collaboration with a Computer Science and Engineering student, creating a bidirectional learning model. I provided clinical and imaging insight, while the student supported Python programming and machine-learning workflows. Over time, I learned to critically understand and evaluate the entire AI pipeline, demonstrating the power of interdisciplinary teamwork in modern medical physics research.
Integrating Imaging and Clinical Data
The final workflow integrated CT-based deep radiomics with clinical biomarkers such as HPV/p16 status, smoking history, TNM stage, and tumor volume. Survival modeling was performed using Cox-based neural networks to predict overall and disease-free survival. Regular mentor meetings ensured both methodological rigor and clinical relevance.
Impact of GREMP
GREMP reshaped my professional identity. I learned to critically assess AI literature, understand uncertainty and bias in predictive models, and collaborate across disciplines. Most importantly, I realized that one does not need to begin as an AI expert to contribute meaningfully to AI-driven medical physics.
By providing research mentorship to LMIC physicists, GREMP provides an equitable and scalable model for global research capacity building. With structured mentorship and collaborative learning, advanced data-driven research is achievable even in resource-limited settings.

Radiopharmaceutical Therapy: Current Trends and Clinical Trial Landscape
Senthamizhchelvan Srinivasan
Department of Radiation Oncology, Indiana University, Indianapolis, IN, USA
Abstract:
Radiopharmaceutical therapy (RPT), also referred to as radioligand or targeted radionuclide therapy, has rapidly evolved from a niche salvage option into a central pillar of precision oncology. The field is driven by the success of lutetium-177 based agents in neuroendocrine tumors (NETs) and prostate cancer, the maturation of alpha-emitting therapies, and the emergence of new targets such as fibroblast activation protein (FAP). Recent analyses describe about 30 active phase III trials, with neuroendocrine, prostate, and thyroid cancers representing nearly three-quarters of late-stage development. Concurrently, the global radioligand therapy market is projected to reach roughly USD 13 billion by 2030. This review summarizes key trends in approved and emerging radiopharmaceuticals, highlights pivotal clinical trials across major disease areas, and discusses technical, regulatory, and infrastructure considerations that will shape RPT integration into routine cancer care.
1. Introduction
Radiopharmaceutical therapy combines a radionuclide “warhead” with a tumor-targeting vector commonly a peptide, small molecule, or antibody to deliver ionizing radiation selectively to malignant tissue. Historically, RPT was largely limited to iodine-131 for differentiated thyroid cancer and bone-targeted agents such as strontium-89 or samarium-153. Over the last decade, three landmark phase III trials ALSYMPCA (radium-223), NETTER-1 (177Lu-DOTATATE), and VISION (177Lu-PSMA-617) provided high-level evidence and led to regulatory approvals that transformed the perception of RPT from experimental to mainstream.
A 2025 minireview of phase III RPT trials identified 34 active phase III studies, with neuroendocrine tumors, prostate cancer, and differentiated thyroid carcinoma accounting for nearly 75% of trials. In parallel, an industry analysis in Nature Reviews Drug Discovery reported two currently marketed “new-generation” radioligand therapies and 60-plus additional RPTs in clinical development across a broad range of solid and hematologic malignancies. Economically, recent market reports estimate that the radioligand therapy segment was approximately USD 9.2 billion in 2024 and is expected to grow to about USD 13–13.8 billion by 2030. Growth is fueled by increasing cancer incidence, expanding indications for approved agents, and a robust late-stage pipeline.
2. Approved Radiopharmaceutical Therapies and Core Platforms
2.1 Established Agents
Key approved RPTs include:
- 177Lu-DOTATATE (Lutathera®) – peptide receptor radionuclide therapy (PRRT) targeting somatostatin receptor 2, approved for SSTR-positive gastroenteropancreatic NETs based on NETTER-1.
- 177Lu-PSMA-617 (Pluvicto®) – PSMA-targeted small-molecule radioligand therapy for metastatic castration-resistant prostate cancer (mCRPC), initially approved post-taxane based on VISION and subsequently expanded (see below).
- 223RaCl₂ (Xofigo®) – alpha-emitting agent targeting bone metastases in mCRPC.
- 131I (radioiodine) – long-established metabolic therapy for differentiated thyroid cancer, now being refined rather than replaced.
Therapeutic platforms span radiolabeled peptides (PRRT), small-molecule ligands (PSMA, FAP, CXCR4), monoclonal antibodies, and intra-arterial microspheres (e.g., 90Y-labeled glass or resin microspheres) for liver-directed therapy.
2.2 Expansion of Pluvicto into Earlier mCRPC
On March 28, 2025, the U.S. FDA expanded the indication of lutetium Lu-177 vipivotide tetraxetan (Pluvicto) to include adults with PSMA-positive mCRPC previously treated with one androgen receptor pathway inhibitor (ARPI) and deemed appropriate to delay taxane-based chemotherapy.
- The phase III PSMAfore trial randomized 468 patients with PSMA-positive mCRPC progressing on one ARPI to Pluvicto or ARPI switch. Median radiographic PFS was 9.3 vs 5.6 months (HR 0.41), favoring Pluvicto, with a strong trend but non-significant difference in overall survival in the intention-to-treat analysis.
- Novartis reports an updated analysis showing more than a doubling of median rPFS (~11.6 vs 5.6 months) and an OS benefit after adjustment for crossover.
- This label expansion effectively moves radioligand therapy into a pre-chemotherapy setting in mCRPC and is estimated to triple the eligible U.S. patient population.
Guideline-level frameworks for Lu-PSMA use have been published by the Society of Nuclear Medicine and Molecular Imaging (SNMMI) and joint EANM/SNMMI procedure guidelines. These documents define patient selection criteria (PSMA PET positivity, prior therapies), safety monitoring, and scenarios for off-label use.
3. Market and Industrial Landscape: From Niche to Pillar
Several converging trends underscore that RPT is becoming a durable modality rather than a transient niche:
- Pipeline depth: The 2025 landscape overview counts about 67 radioligand products in clinical development, encompassing a wide variety of targets (PSMA, SSTR, FAP, HER2, TROP2, CD38, CD20, CXCR4, and others).
- Market growth: Independent market analyses project the global radioligand therapy market at USD 13–13.8 billion by 2030, with growth concentrated in prostate cancer and NET indications and rapid uptake in Asia-Pacific.
- Industrial investment: In November 2025, Novartis opened a 10,000-sq-ft radioligand manufacturing facility in Carlsbad, California, as part of a USD 23 billion U.S. expansion plan, specifically to stabilize and accelerate supply of Pluvicto and Lutathera for the western U.S.
Because many therapeutic radionuclides have short half-lives and are often produced in single-patient batches, the field depends on reliable isotope production, regional manufacturing hubs, and robust cold-chain logistics.
4. Disease-Specific Trends and Pivotal Clinical Trials
4.1 Neuroendocrine Tumors (NETs)
4.1.1 PRRT in Earlier-Line GEP-NETs
Following NETTER-1, which established 177Lu-DOTATATE plus octreotide as a standard in progressive midgut NETs, recent trials are pushing PRRT into earlier lines and higher-grade disease.
- NETTER-2 (NCT03972488): In untreated, well-differentiated grade 2–3 GEP-NETs (Ki-67 10–55%), adding 177Lu-DOTATATE to standard-dose octreotide nearly tripled median PFS (22.8 vs 8.5 months) and reduced risk of progression or death by ~72% vs high-dose octreotide alone.
- COMPOSE (NCT04919226): Compares 177Lu-DOTATOC with everolimus in progressive GEP-NETs, with recruitment completed and results pending.
- COMPETE (NCT03049189): Has completed accrual and will compare PRRT directly with everolimus in GEP-NETs.
These data support a shift toward first-line or early-line PRRT in selected patients with high-burden or higher-grade well-differentiated NETs, although long-term overall survival and health-economic outcomes will be crucial to guideline adoption.
4.1.2 Personalised Dosimetry
Because PRRT produces heterogeneous intratumoral dose distributions, fixed activities can yield widely variable absorbed doses between patients.
- The STARTNET trial (NCT05387603) randomizes patients to standard 4 × 7.5 GBq 177Lu-DOTATOC vs individualized dosimetry-guided dosing based on dual 68Ga-DOTATOC and 18F-FDG imaging, with outcomes including efficacy, toxicity, and cost.
This aligns with IAEA and JNM initiatives emphasizing patient-specific dosimetry and quantitative SPECT/CT as a route to true theranostic personalization.
4.1.3 Emergence of Alpha PRRT
To improve tumor kill in resistant disease, alpha-emitting isotopes such as actinium-225 are being evaluated:
- ACTION-1 (NCT05477576): A global phase 1b/3 trial of 225Ac-DOTATATE (RYZ101) vs standard of care in SSTR-positive GEP-NETs progressing after 177Lu-PRRT. Early phase 1b data show encouraging dosimetry and tolerability without dose-limiting toxicities.
If successful, ACTION-1 may establish alpha-PRRT as a salvage or even preferred approach in patients failing lutetium-based therapy.
4.2 Prostate Cancer
Prostate cancer is the most mature non-thyroid indication for RPT, dominated by PSMA-targeted therapies.
4.2.1 Lu-PSMA in mCRPC and Earlier Disease
Beyond VISION and the PSMAfore-driven label expansion discussed above, further trials are exploring:
- 177Lu-PSMA-I&T: Two phase III trials in mCRPC (NCT04647526, NCT05204927) have completed recruitment and will determine whether this widely used “compassionate-use” compound achieves registrational status.
- Earlier-stage disease: At least five phase III studies are evaluating 177Lu-PSMA-617 in:
- Metastatic hormone-sensitive prostate cancer (mHSPC) e.g. PSMAddition (NCT04720157) and other trials in mHSPC.
- Oligometastatic settings (e.g., NCT05939414).
A recent Reuters report on a phase III trial in metastatic hormone-sensitive disease noted that Pluvicto significantly slowed disease progression when combined with hormone therapy, reinforcing prospects for pre-mCRPC indications.
4.2.2 Consensus Guidelines and Real-World Use
The SNMMI consensus statement on patient selection and appropriate use of 177Lu-PSMA-617 and the joint EANM/SNMMI procedure guideline have provided detailed criteria on PSMA PET imaging requirements, prior systemic therapy, performance status, and toxicity management. These guidelines are accelerating standardization of RLT outside clinical trials, particularly in the United States and Europe.
4.2.3 Alpha PSMA Therapy
The next wave in prostate RPT involves alpha-emitting PSMA ligands:
- FPI-2265 (225Ac-PSMA-I&T, AlphaBreak; NCT06402331): Is a phase II, randomized, open-label trial optimizing dose and schedule in PSMA-positive mCRPC. The study aims to define a recommended regimen based on safety, tolerability, and antitumor activity, and the first patient has already been dosed.
- Alpha-PSMA agents may offer higher linear energy transfer and shorter path length, potentially overcoming resistance to beta-PSMA therapies while raising new questions about marrow and kidney toxicity.
4.3 Differentiated Thyroid Cancer: Refining Radioiodine Use
Radioiodine has been used for more than 70 years in differentiated thyroid cancer (DTC), but optimal indications and doses remain under evaluation.
4.3.1 ESTIMABL2: De-escalating RAI in Low-Risk DTC
The ESTIMABL2 phase III trial (NCT01837745) randomized low-risk DTC patients to postoperative 131I ablation vs surveillance after total thyroidectomy.
- Five-year results showed non-inferior event-free survival with surgery alone (94% in both arms), indicating no loss of oncologic opportunity when omitting RAI in carefully selected low-risk patients.
These data support restricting radioiodine in low-risk DTC and concentrating its use in higher-risk or metastatic disease.
4.4 Liver Tumors and Pediatric Malignancies
4.4.1 Hepatocellular Carcinoma (HCC): 90Y Microspheres
While radioembolization with 90Y microspheres has been used for years, high-level randomized evidence has been relatively sparse.
- MANDARIN (NCT05016245) is a multicenter, prospective phase III trial in China comparing TheraSphere™ 90Y glass microspheres to conventional TACE in inoperable HCC (China liver cancer stages Ib–IIb). The study is active, with an estimated completion around 2026.
MANDARIN will help clarify whether 90Y radioembolization should be preferred to TACE in intermediate-stage HCC, at least in selected populations.
4.4.2 High-Risk Neuroblastoma: 131I-MIBG and ALK Inhibition
In pediatric oncology, 131I-metaiodobenzylguanidine (MIBG) is an established targeted agent for neuroblastoma. Current studies are incorporating it earlier:
- NCT03126916: A phase III trial testing 131I-MIBG or lorlatinib plus intensive multimodal therapy in newly diagnosed high-risk neuroblastoma/ganglioneuroblastoma.
The trial compares standard therapy and these additions, aiming to improve survival while carefully monitoring late effect. This study exemplifies broader efforts to integrate RPT into frontline pediatric regimens where biologically targeted radiation may complement chemotherapy, surgery, and external beam radiotherapy.
4.5 Fibroblast Activation Protein (FAP)–Targeted Radioligand Therapy
FAP is a type II transmembrane serine protease highly expressed on cancer-associated fibroblasts in the stroma of more than 90% of epithelial cancers, including pancreatic, colorectal, breast, and lung tumors. The success of FAPI-based PET imaging has established FAP as a “pan-tumor” theranostic target.
Recent reviews provide an overview of clinical advances in FAP-targeted radioligand therapy (FAP-RLT):
- Early quinoline-based agents (e.g., FAPI-04, FAPI-46) demonstrated high tumor uptake but short tumor retention, limiting therapeutic efficacy when labeled with beta-emitters.
- Next-generation ligands incorporate albumin-binding moieties, cyclic peptides, or dimeric designs to prolong tumor retention and improve tumor-to-organ dose ratios (e.g., FAP-2286, EB-FAPI, (SA.FAPi)₂, 3BP-3940).
- Early phase clinical data with 90Y-FAPI-46 report manageable hematologic toxicity and disease control (PR+SD) in roughly half of heavily pretreated patients, with strongest signals seen in sarcoma and solitary fibrous tumor.
Currently, FAP-RLT remains early-phase, with multiple trials in pancreatic ductal adenocarcinoma, colorectal cancer, sarcoma, and other stromal-rich tumors. Well-designed randomized trials will be needed to clarify its comparative value versus chemotherapy, external beam radiotherapy, and immunotherapy.
4.6 Emerging Targets Beyond SSTR, PSMA, and FAP
The RLT pipeline is expanding across a range of targets already familiar from monoclonal antibody and ADC development:
- HER2, HER3, and EGFR – radiolabeled antibodies and small molecules are being tested in breast, gastric, and other HER-driven cancers.
- CXCR4: a 2025 preclinical/early translational report on 177Lu-DOTA-CXCR4 highlights favorable biodistribution with reduced liver and kidney uptake compared with some prior CXCR4 agents, supporting its potential as a theragnostic agent for hematologic and solid tumors.
- Other immune and stromal targets (e.g., CD38, CD20, TROP2) are being radiolabeled in exploratory programs, often aiming for synergistic combinations with checkpoint inhibitors or established systemic therapies.
5. Radionuclide Science: Lutetium Dominance and Alpha Expansion
5.1 Lutetium-177 as the Workhorse
The Frontiers overview notes that 177Lu is used in 17 of 34 active phase III RPT trials and in more than 200 ongoing studies overall, reflecting its favorable half-life (~6.7 days), beta energy, and co-emitted gammas enabling post-therapy imaging. Recent work on 177Lu-based therapy emphasizes:
- Optimization of patient-specific dosimetry, moving beyond fixed activities to individualized treatment courses.
- Development of new carrier molecules and bifunctional chelators under IAEA-sponsored coordinated research projects.
5.2 Targeted Alpha Therapy (TAT)
Alpha-emitters such as 225Ac, 211At, 212Pb/212Bi, 223Ra, 149Tb, and 227Th deliver high-LET radiation over a very short path length, potentially enhancing tumor cell kill while sparing surrounding healthy tissue. Key trends in TAT include:
- Clinical maturation in NETs and prostate cancer, exemplified by ACTION-1 (225Ac-DOTATATE) and AlphaBreak (225Ac-PSMA-I&T).
- Renewed efforts to solve production and supply challenges for alpha emitters, particularly 225Ac, which historically has been limited by generator capacity and cost.
A 2024 review in European Journal of Nuclear Medicine and Molecular Imaging underscores broad interest in TAT across brain tumors, bladder cancer, leukemia, NETs, and prostate cancer, while cautioning that toxicity profiles, dosimetry, and long-term safety remain incompletely defined.
6. Dosimetry, Quality Assurance, and Regulatory Initiatives
6.1 Toward Routine Patient-Specific Dosimetry
Modern RPT is moving from empiric dosing towards quantitative, individualized planning:
- The IAEA monograph “Dosimetry for Radiopharmaceutical Therapy” and related coordinated research projects promote standardized methods for SPECT/CT-based activity quantification, time–activity curve fitting, and absorbed dose estimation.
- JNM reviews emphasize that dosimetry can optimize tumor control while respecting organ-at-risk constraints, but implementation varies widely between centers and software platforms.
- Trials such as STARTNET will provide critical prospective evidence for whether dosimetry-guided PRRT improves outcomes compared with simple fixed-activity regimens.
6.2 Operational Readiness and Quality Assurance
Implementing RPT requires:
- Reliable radionuclide supply, hot-lab infrastructure, and radiation safety protocols.
- Multidisciplinary teams (nuclear medicine, medical physics, nursing, pharmacy, oncologists) trained in handling unsealed sources and managing therapy-specific toxicities.
- Center-level quality assurance programs to ensure accurate activity calibration, imaging quantification, and record-keeping for regulatory compliance.
- Regulatory and professional bodies (e.g., SNMMI, EANM, IAEA) increasingly provide guidance on appropriate use criteria, dosimetry standards, and clinical trial design, helping to harmonize practice across regions.
7. Future Directions and Conclusions
Radiopharmaceutical therapy is entering what many have called its “third wave”:
- Expansion of approved indications: earlier-line use of 177Lu-PSMA-617 in mCRPC and likely in mHSPC, and first-line PRRT for selected higher-grade GEP-NETs (NETTER-2).
- New targets and tumor types: FAP-RLT, CXCR4, HER2/HER3, and others broaden RPT beyond NETs and prostate cancer, with pan-tumor theranostic strategies under active investigation.
- Technical differentiation: alpha-emitters, innovative chelators, and sophisticated dosimetry may allow therapies to be tailored according to tumor biology, spatial disease distribution, and patient-specific radiobiology.
- System-level integration: large-scale investments in manufacturing (e.g., Novartis’s Carlsbad facility and U.S. expansion) and maturing regulatory frameworks indicate that RPT is being treated as a strategic long-term modality rather than a niche.
For clinicians and trialists, the implications are clear:
- Oncology teams should anticipate earlier referral points for PRRT and Lu-PSMA therapies and consider clinical trial enrollment as part of first or second-line treatment pathways.
- Nuclear medicine and medical physics units need to invest in dosimetry capabilities, QA, and multidisciplinary training to meet increasing demand.
- Health systems and payers must plan for the cost and logistical complexity of RPT while recognizing its potential to improve progression-free survival, quality of life, and, in some settings, overall survival.
As of late 2025, radiopharmaceutical therapy is firmly established as a critical component of precision oncology, with the next decade likely to bring more indications, more isotopes, and more personalized treatment paradigms.
References
- Lepareur N. An overview of current phase 3 radiopharmaceutical therapy clinical trials. Front Med. 2025;12:1549676.
- To J, et al. The landscape for radioligand therapies in oncology. Nat Rev Drug Discov. 2025;24:584–585.
- Meditech Insights. Radioligand Therapy Market Size, Industry Growth, Trends, Analysis and Forecast to 2030. 2023–2025 update.
- P&S Intelligence. Radioligand Therapy Market Size and Growth Forecast 2019–2030.
- U.S. FDA. FDA expands Pluvicto’s metastatic castration-resistant prostate cancer indication. March 28, 2025.
- Novartis. FDA approves Novartis radioligand therapy Pluvicto® for earlier use before chemotherapy in PSMA-positive metastatic castration-resistant prostate cancer. Media release, 28 March 2025.
- Singh S, et al. NETTER-2 primary analysis; reported in: The ASCO Post February 25, 2024.
- NETRF. NETTER-2 Trial Shows Lutathera® as First-Line Treatment Significantly Reduces Disease Progression or Death. January 22, 2024.
- Hope TA, et al. SNMMI Consensus Statement on Patient Selection and Appropriate Use of 177Lu-PSMA-617 Radionuclide Therapy. J Nucl Med. 2023;64(9):1417–1423.
- Kratochwil C, et al. and related TAT reviews summarized in: Eychenne R, et al. Overview of the Most Promising Radionuclides for Targeted Alpha Therapy: The “Hopeful Eight”. Pharmaceutics. 2021;13:906.
- Wu X, et al. Recent clinical advances in fibroblast activation protein targeted radioligand therapy for solid tumors. Front Nucl Med. 2025.
- Kang YK. Fibroblast Activation Protein-Targeted Theranostics: Current Status in Clinical Development. Nucl Med Mol Imaging. 2025;59:279–288.
- Hobbs RF, Bardiès M. Dosimetry in Radiopharmaceutical Therapy. J Nucl Med. 2022;63(10):1467–1477.
- Sathekge, M., Morgenstern, A. Advances in targeted alpha therapy of cancer. Eur J Nucl Med Mol Imaging 51, 1205–1206 (2024).
- IAEA. Dosimetry for Radiopharmaceutical Therapy. IAEA, 2023.
- ESTIMABL2 collaborators. Five-year analysis summarized in: Lancet Diabetes Endocrinol 2024 and secondary reports.
- ClinicalTrials.gov and associated registries for NCT05387603 (STARTNET), NCT05477576 (ACTION-1), NCT05016245 (MANDARIN), NCT03126916 (high-risk neuroblastoma), NCT05468554 (METHYR), NCT06402331 (AlphaBreak), among others.

SCMPCR E-Learning Program (ELP-10): Soft Skills for Medical Physicists and Scientists in Cancer Research
1,2Mohamaad Ullah Shemanto, 1Md. Jabidul Islam
1South Asia Centre for Medical Physics & Cancer Research (SCMPCR)
2Evercare Hospital Chattogram
The South Asia Centre for Medical Physics and Cancer Research (SCMPCR) successfully conducted its 10th E-Learning Program (ELP-10) from 1 to 21 November 2025. Titled “Soft Skills for Medical Physicists and
Scientists in Cancer Research,” the program integrated professional development with technically advanced topics essential for modern cancer care.

Accredited by the European Board for Accreditation in Medical Physics (EBAMP), the course awarded up to 35 Continuing Professional Development (CPD) points. The program achieved significant global reach, attracting 62 participants from 22 countries across South Asia, Southeast Asia, the Middle East, Europe, Africa, and Australia.
Day 02: Three-Dimensional Printing in Radiotherapy
Speaker:Mr. Timothy Froese, Director of Commercial Strategy, Adaptive Medical Technologies, Halifax, Canada.
Moderator: Dr. Md. Akhtaruzzaman, Chief Medical Physicist and Radiation Safety Officer, Evercare Hospital Chattogram, Bangladesh.
Mr. Froese led the session, moderated by Dr. Md. Akhtaruzzaman. It demonstrated how additive manufacturing integrates into radiotherapy workflows for patient-specific bolus design, immobilization, and QA phantoms. The discussion highlighted innovative, cost-effective solutions applicable to resource-limited settings.
Day 03: Artificial Intelligence in Radiation Medicine
Speaker:Dr. Hannah Mary Thomas T, Staff Scientist and DBT–Welcome India Alliance Early Career Fellow, Biomedical Informatics Unit, Christian Medical College, Vellore, India.
Moderator: Mohammad Ullah Shemanto, Medical Physicist, Evercare Hospital Chattogram, Bangladesh.
Dr. Hannah delivered a comprehensive overview of AI applications, moderated by Mohammad Ullah Shemanto. The lecture covered image segmentation, outcome prediction, and workflow automation. Participants gained clarity on data requirements, validation, bias, and interpretability to better engage with research literature.
Day 04: Digital Medical Image Processing Techniques
Speaker:Prof. Dr. med. Thomas Schrader, Expert in Medical Informatics, Department of Informatics and Media, Brandenburg University of Applied Sciences, Germany.
Moderator: Md. Motiur Rahman (Mithu), Chief Medical Physicist & Assistant Project Director TMSS Cancer Centre (TCC).
Prof. Thomas Schrader focused on image filtering, feature extraction, and quantitative analysis, with Md. Motiur Rahman moderating. The session established clear links between digital processing, radiomics, adaptive radiotherapy, and imaging-based biomarkers in cancer research.
Day 05: Clinical Implementation of PSQA Software and SGRT Systems
Speaker:Mr. Maximilian Grohmann, Medical Physicist, Department of Radiotherapy and Radiation Oncology, University Medical Center Hamburg-Eppendorf, Germany &
Dr. Hui Khee Looe, Deputy Head, Department of Medical Physics, Pius-Hospital, Oldenburg, Germany.
Moderator: Dr. Anwarul Islam, Coordinator Medical Physicist, Square Hospitals Ltd, Dhaka, Bangladesh.
Mr. Maximilian Grohmann and Dr. Hui Khee Looe presented practical strategies for commissioning and workflow integration, moderated by Dr. Anwarul Islam. Participants reviewed early clinical experiences and safety considerations necessary for implementing patient-specific QA and surface-guided radiotherapy systems.
Day 06: Practical Leadership Skills for Junior Physicists
Speaker:Prof. Dr. Carmel J. Caruana, Head, Department of Medical Physics, University of Malta, Msida, Malta.
Moderator: Meher Nigar Sharmin, Medical Physicist, Khwaja Yunus Ali Medical College and Hospital (KYAMCH Cancer Center), Enayetpur, Sirajganj, Bangladesh.
Prof. Caruana addressed leadership, communication, and career development, with Meher Nigar Sharmin moderating. The session emphasized the growth of soft skills alongside technical expertise within clinical and academic environments.
Day 07: From Submission to Publication
Speaker:Prof. Dr. Iuliana Toma-Dasu, Head of Medical Radiation Physics, Department of Physics, Stockholm University, Sweden, and Chief Editor of Physica Medica.
Moderator: Ms. Bushra Intakhab, Department of Physics, Florida Atlantic University, USA.
Prof. Toma-Dasu provided practical insights into manuscript preparation and peer review expectations, moderated by Ms. Bushra Intakhab. The discussion covered common rejection reasons and ethical reporting to support participants’ research and publication efforts.
Day 08: Optimization and Score Functions in Radiotherapy
Speaker:Dr. Phil W. Koken, Medical Physicist, Department of Radiation Oncology, Amsterdam UMC, Netherlands.
Moderator: Dr. Md. Alamgir Kabir, Associate Professor, Department of Physics, Jahangirnagar University, Savar, Dhaka.
Dr. Phil explored objective functions and trade-offs in inverse planning, moderated by Dr. Md. Alamgir Kabir. The session strengthened participants’ ability to critically interpret treatment plans by highlighting the limitations of automated optimization.
Day 09: Group Discussion and Interactive Exchange
The program concluded with a dynamic forum moderated by Dr. Raju Srivastava and Dr. Mary Joan, who also serves as Co-Editor-in-Chief of the SCMPCR Newsletter. This session allowed for direct, enthusiastic dialogue between participants, faculty, and a representative from LAP regarding vendor-specific inquiries. By addressing clinical challenges and research barriers in real-time, the exchange fostered peer learning and international collaboration, effectively bridging the gap between theoretical knowledge and practical professional growth.
Participant Evaluation and Feedback
Evaluations indicated high satisfaction with the program’s organization and its balance between technical depth and professional development. Participants specifically noted increased confidence in utilizing Monte Carlo methods, AI, and modern QA systems. While the leadership and publication-focused sessions were highly valued for addressing professional challenges, constructive feedback suggested adding more hands-on components and case-based discussions in future iterations to further enhance the learning experience.
Examination Outcomes and Recognition of Excellence
A formal online examination on 21 November 2025 resulted in an impressive average score of 84.7% (33/40). Top honors with a score of 38/40 were awarded to Ayesha Nur, Bushra Intakhab, and Sakhi Sara. Second-place honors (37/40) went to Morium Akter, Ahlam Azalmad, Saloni Chawla, Sheikh Faysal, Haritha Karunarathne, Suresh Poudel, and Sumaya Sumaya. Third-place (36/40) was shared by Safwan Araf Alvey, Jose Luis Paolo Domingo, and Md. Mokhlesur Rahman. These results confirm effective knowledge transfer across the diverse global cohort.
Mentorship and Ongoing Engagement
To foster future leadership, top-ranked participants have been invited to serve as SCMPCR Moderators and Ambassadors. A dedicated mentorship group has been established to provide ongoing academic guidance and pathways for active involvement in research and outreach. This initiative aims to transform academic success into long-term professional contributions, ensuring a sustained global network of skilled medical physicists.
Conclusion
ELP-10 successfully integrated advanced technical training with essential soft skills, supporting the professional readiness of medical physicists worldwide. SCMPCR remains committed to providing inclusive, high-quality education that empowers scientists to lead innovation and ensure safe clinical practice in global cancer care.

The Future of SCMPCR: Building Capacity in Medical Physics and Cancer Care in South Asia
Bushra Intakhab
Department of physics, Florida Atlantic University, Boca Raton, USA
Introduction
The South Asia Centre for Medical Physics and Cancer Research (SCMPCR) has emerged as a leading regional platform dedicated to strengthening cancer care, education, and research across South Asia. Since its establishment, SCMPCR has focused on addressing the growing demand for trained medical physicists, radiation professionals, and healthcare workers through structured education, hands on training, and community-based awareness programs.
Cancer remains one of the leading causes of death in low- and middle-income countries. Limited access to trained professionals, modern technology, and continuous education remains a major challenge. SCMPCR was founded with the vision of reducing this gap by creating a sustainable ecosystem of education, training, and professional development in medical physics and radiation sciences.
Vision and Mission
The long-term vision of SCMPCR is to become a regional center of excellence for education, research, and capacity building in medical physics and cancer care.
Mission Objectives
- To provide high-quality education and training in medical physics and radiation sciences
- To develop skilled professionals capable of delivering safe and effective cancer care
- To promote research, innovation, and international collaboration
- To strengthen healthcare systems through structured training programs
- To support cancer awareness, prevention, and early detection initiatives
Key Program Areas of SCMPCR
SCMPCR operates through multiple structured programs designed to meet different educational and professional needs.
1. Hands-on Training Programs
Hands-on workshops focus on practical learning in clinical environments. These programs emphasize:
- Radiotherapy quality assurance
- Dosimetry and treatment planning
- Imaging and treatment verification
- Practical exposure to modern radiotherapy equipment
- These workshops are conducted in collaboration with national and international hospitals and universities.
2. E-Learning Programs (ELP)
SCMPCR launched its e-learning platform to expand access to education globally. These programs allow professionals to learn without geographical barriers.
Key features includes:
- Live interactive lectures
- Expert-led sessions from global institutions
- Recorded content and study materials
- Assessment and certification
E-learning programs cover topics such as:
- Medical physics
- Radiation oncology
- Brachytherapy
- Diagnostic imaging
- Radiation safety and quality assurance
3. In-Service Training Programs
These programs are designed for professionals already working in hospitals.
Training is conducted within healthcare facilities to strengthen practical skills in real clinical environments. Focus areas include:
- Equipment commissioning
- Quality control and assurance
- Clinical workflow optimization
- Safety protocols
4. Awareness and Community Outreach
SCMPCR actively conducts cancer awareness programs, especially in underserved and rural regions. These programs focus on:
- Breast and cervical cancer screening
- Early detection and prevention
- Community education and awareness
- Women’s health and public engagement
5. Self-Help and Patient Support Programs
SCMPCR has introduced structured self-help groups for cancer patients. These groups provide:
- Emotional support
- Peer interaction
- Awareness on treatment and recovery
Growth and Impact:
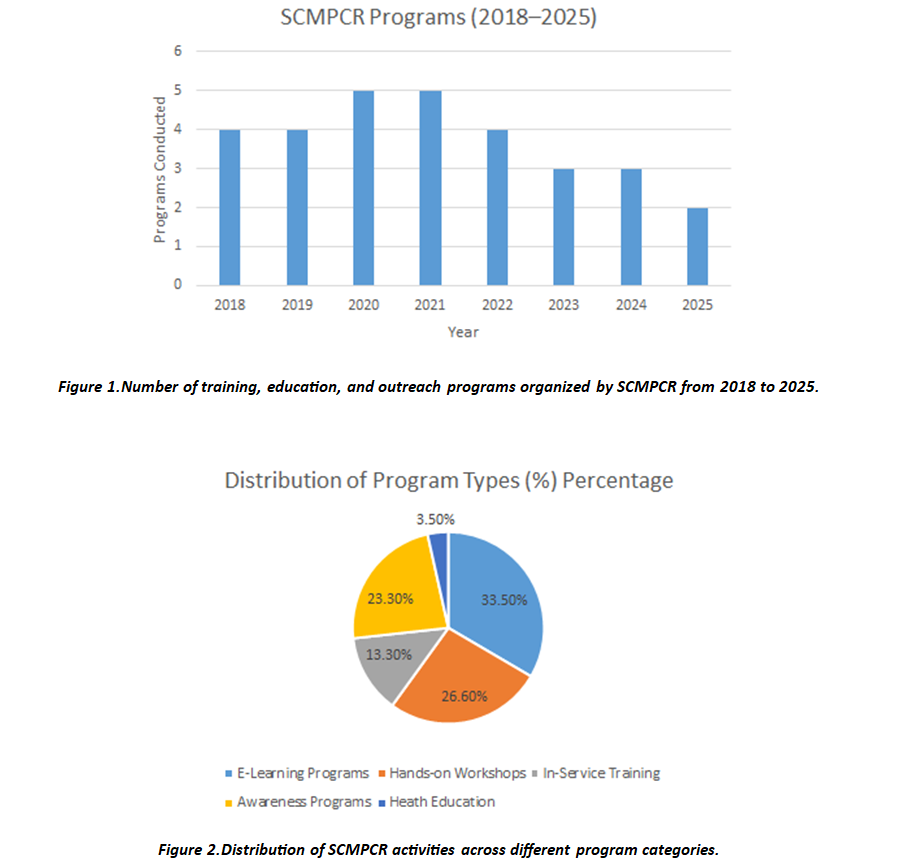
Future Direction of SCMPCR
1. Accredited Learning Programs
SCMPCR plans to establish internationally accredited residency and fellowship programs in:
- Medical Physics
- Radiation Oncology
- Clinical Imaging
- Artificial Intelligence
These programs will align with global accreditation standards and offer structured mentorship.
2. Expansion of Digital Learning Platforms
Future plans include:
- Hybrid learning models
- Virtual simulation based training
- Global expert lecture series
3. Research and Innovation Hub
SCMPCR aims to become a regional research hub by:
- Promoting clinical and translational research
- Supporting young researchers
- Collaborating with international universities
4. Capacity Building in Low-Resource Settings
Special focus will be placed on:
- Rural healthcare facilities
- Training of technicians and technologists
- Mobile screening and diagnostic programs
5. International Collaboration
SCMPCR will strengthen partnerships with:
- Universities and hospitals worldwide
- International professional societies
- Global cancer organizations
Conclusion
SCMPCR continues to play a transformative role in advancing medical physics education, cancer care, and professional development across South Asia.
Through structured training programs, international collaborations, and community-driven initiatives, the organization is shaping a sustainable future for cancer care.
Its commitment to quality education, research excellence, and social responsibility positions SCMPCR as a leading institution in the region and a model for similar initiatives worldwide

The Multifaceted Journey of Dr. Jeyasingam Jeyasugiththan: The Evolving Role of Medical Physicists and Insights for SCMPCR
Mary Joan
Christian Medical College and Hospital, Ludhiana, India
The Multifaceted Journey of Dr. Jeyasingam Jeyasugiththan: The Evolving Role of Medical Physicists and Insights for SCMPCR
The South Asia Centre for Medical Physics and Cancer Research (SCMPCR) is dedicated to strengthening the fields of medical physics and cancer research across South Asia, with the overarching objective of improving patient care and advancing global health. Through a range of structured teaching and training programmes, SCMPCR actively addresses the region-specific challenges faced by medical physicists. What began as a visionary initiative by pioneering leaders has evolved into a phase of dynamic growth, driven by strategic collaborations and meaningful partnerships. Building on these early efforts, SCMPCR has accelerated its progress through innovative and impactful training initiatives.
The SCMPCR Newsletter is one such initiative that celebrates the achievements of medical physicists and highlights ongoing professional activities, fostering sustainable partnerships and collaborative efforts across South Asia.
In this exclusive interview, we have the privilege of interacting with Dr. Jeyasingam Jeyasugiththan, a distinguished medical physicist and nuclear scientist from Sri Lanka, and the first and former Chief Editor of the SCMPCR Newsletter. Currently a Professor in the Department of Nuclear Sciences at the University of Colombo, Sri Lanka, Dr. Jeyasingam has made substantial contributions to academic development, clinical practice, and professional capacity building in medical physics, not only in Sri Lanka and South Asia, but also extending to Papua New Guinea.
In this conversation, Dr. Jeyasingam reflects on his association with SCMPCR, shares insights from his editorial journey, and discusses the organisation’s growth and its pivotal role in advancing medical physics and cancer research. He also offers expert perspectives on the evolving landscape of medical physics, highlighting technological advances alongside persistent regional challenges. Presented below is a curated excerpt from the discussion between Dr. Mary Joan (MJ) and Dr. Jeyasingam Jeyasugiththan (JJ), focusing on his contributions and involvement in establishing SCMPCR activities.

MJ: Glad to have this opportunity to hear from you. Could you please share your early experiences and what motivated you to pursue medical physics as a career?
JJ: I initially studied physics at the undergraduate level, where I developed a strong interest in its medical applications. During my master’s programme in medical physics, I gained a deeper understanding of how fundamental physics principles could be directly applied to improve human health. This experience strongly motivated me to pursue medical physics as my professional career.
While I was completing my MSc in Medical Physics, there was a proposal to establish a cancer treatment centre in Jaffna, Sri Lanka. At that time, Prof. Nagalingam Suntharalingam from the USA, widely known as Prof. Suntha was working closely with the provincial government to support the establishment of this centre at Tellippalai Base Hospital. Through a colleague, I was introduced to Prof. Suntha, as the hospital required a medical physicist. Following several discussions with him and the Regional Directorate of Health Services, Jaffna, I was appointed as a contract Medical Physicist in 2005 and later confirmed as a permanent Medical Physicist in 2016.
Prof. Suntha also arranged three months of clinical training for me in India under the supervision of Prof. Paul Ravindran at Christian Medical College, Prof. Challapalli Srinivas at Kasturba Medical College, and Prof. Thayalan at Chennai Medical College.
Over the next 14 years, I worked as a clinical medical physicist and played a key role in establishing medical physics services at Tellippalai Base Hospital and Jaffna Teaching Hospital.
Subsequently, I was awarded the opportunity to pursue my PhD at the University of Cape Town, where I conducted my research at the iThemba LABS proton beam facility. After completing my PhD, I joined the Department of Nuclear Sciences at the University of Colombo as an academic medical physicist. Alongside my academic role, I continue to contribute clinically by training and mentoring junior medical physicists and teaching at the master’s and doctoral levels.
MJ: You have personally nurtured many collaborations for SCMPCR. Could you enlighten us on the early status of the organisation and the challenges faced?

JJ: During the early stages of SCMPCR, collaboration was both our greatest strength and our most significant challenge. The centre was still developing its identity, and many medical physicists in the region were not fully aware of SCMPCR or its objectives. One of the main challenges was connecting professionals across different countries, institutions, and clinical settings, particularly when resources, infrastructure, and training opportunities varied considerably across South Asia.
Another major challenge was limited funding and logistical support, especially from countries such as Sri Lanka. In recent years, Sri Lanka experienced a severe economic crisis following the COVID-19 pandemic. As a result, many SCMPCR activities relied heavily on voluntary contributions, personal networks, and the dedication of a small group of committed professionals.
Despite these constraints, there was a strong shared vision among the founding members to improve education, training, and research in medical physics and cancer care across the region. Building trust and long-term partnerships took time, but through regular interactions, workshops, newsletters, and academic exchanges, SCMPCR gradually gained recognition and credibility.
These early challenges helped shape SCMPCR into a resilient and collaborative organisation and reinforced the importance of teamwork, regional cooperation, and sustained commitment, principles that continue to guide its activities today.
MJ: Your contributions have shaped the SCMPCR Newsletter into what it is today. Could you share how you overcame the challenges you faced and your thoughts on its future prospects?
JJ: Developing the SCMPCR Newsletter was both challenging and highly rewarding. In the initial stages, one of the main difficulties was ensuring regular contributions while maintaining consistent quality, particularly with very limited resources. Many contributors were busy clinicians or academics, and coordinating content and meeting deadlines required persistence and continuous engagement.
I addressed these challenges primarily through teamwork and direct communication. By encouraging young medical physicists, reaching out to senior professionals, and building trust within the community, we were able to create a platform where contributors felt motivated to share their work and experiences. Strong support from SCMPCR leadership and regional collaborators was also crucial in sustaining the newsletter.
Looking ahead, I envision the SCMPCR Newsletter evolving into a more interactive and regionally inclusive platform. It has significant potential to highlight research activities, training opportunities, and success stories across South Asia, while also fostering collaboration with international partners. With continued commitment and effective leadership, the newsletter can further strengthen the medical physics community and support SCMPCR’s long-term goals.
MJ: How do you view the current professional scenario for medical physicists in South Asia?
JJ: The professional landscape for medical physicists in South Asia reflects both encouraging progress and ongoing challenges. On the positive side, there is increasing recognition of the critical role played by medical physicists, particularly in diagnostic imaging. Many countries in the region are expanding radiotherapy and imaging services, which has led to a growing demand for trained professionals.
However, disparities persist across countries in terms of training standards, availability of equipment and funding, career recognition, and opportunities for professional development. In certain regions, medical physicists face limited career progression and a lack of structured continuing education programmes.
Despite these challenges, the outlook remains optimistic. Regional organisations such as SCMPCR, in collaboration with universities and international agencies, are making meaningful contributions to education, training, and professional networking. With sustained regional cooperation, standardised training pathways, and robust professional support, the role of medical physicists in South Asia will continue to expand and strengthen.
MJ: Could you share some of your most memorable experiences from your collaborations with SCMPCR?
JJ: My most memorable experiences with SCMPCR stem from the strong sense of teamwork and shared purpose. Collaborating with colleagues from different South Asian countries each facing unique challenges yet offering distinct strengths was both inspiring and fulfilling.

One particularly memorable aspect was the early development of the SCMPCR Newsletter. Bringing together contributions from clinicians, academics, and early-career professionals created a shared platform for communication and learning. Witnessing the enthusiasm of young medical physicists, especially when their work was acknowledged and published, was deeply encouraging.
I also value the collaborations developed through SCMPCR training programmes, workshops, and academic exchanges. These initiatives not only enhanced professional skills but also fostered lasting professional relationships built on trust and mutual respect. Overall, my experiences with SCMPCR have been profoundly meaningful, demonstrating the power of regional collaboration in advancing medical physics and improving patient care.
MJ: What future prospects should medical physicists in South Asia prepare for?
JJ: Medical physicists in South Asia must prepare for a rapidly evolving professional environment. Emerging technologies, including the integration of artificial intelligence into medicine, are transforming clinical practice. Medical physicists must continuously update their knowledge and skills to ensure safe and effective implementation of these technologies.
There will also be an increasing demand for expertise in radiation dose optimisation, quality assurance, and patient safety, particularly as diagnostic imaging and radiotherapy services continue to expand. Competencies in data analysis, research methodology, programming, and clinical problem-solving will become increasingly important.
Furthermore, medical physicists should be prepared to assume leadership, teaching, and advisory roles within healthcare systems. Regional collaboration, continuous professional development, and adherence to international standards will be essential. By remaining adaptable and committed to lifelong learning, medical physicists in South Asia can play a pivotal role in shaping the future of healthcare.
MJ: What advice would you offer to young medical physicists in South Asia regarding career development?

JJ: My advice to young medical physicists is to build a strong foundation in clinical practice, research, and emerging areas such as artificial intelligence. Always prioritise patient safety, quality assurance, and a clear understanding of how your work directly influences patient outcomes. Research skills are as important as theoretical knowledge.
I strongly encourage continuous learning and staying updated with new technologies, guidelines, and international standards. Take advantage of training programmes offered by SCMPCR, participate in workshops, and engage in online learning. Seeking mentorship from senior professionals within the South Asian region can be extremely valuable.
Networking and collaboration are equally important. Engage actively with regional and international professional organisations such as SCMPCR, attend conferences, and disseminate your work through presentations and publications. Career growth requires patience and perseverance, but with dedication, ethical practice, and teamwork, young medical physicists can build fulfilling careers that meaningfully contribute to healthcare in South Asia.
MJ: SCMPCR is planning to venture into publishing a medical physics journal in the coming years. What groundwork is required before initiating such an endeavour?
JJ: Before launching a medical physics journal, SCMPCR must establish a strong foundation. First, the scope and objectives of the journal should be clearly defined, addressing regional needs while maintaining international scientific standards. A competent and diverse editorial board, comprising experts from South Asia and international collaborators, will be essential.
Second, transparent editorial policies and ethical guidelines must be developed, covering peer-review processes, authorship criteria, and publication ethics. Training editors and reviewers to ensure high-quality and timely peer review will be critical.
In addition, SCMPCR should establish a reliable digital publication platform with efficient manuscript submission and tracking systems. Encouraging high-quality submissions through research training programmes, workshops, and mentorship initiatives will help generate robust content. With careful planning, strong leadership, and community engagement, SCMPCR can successfully establish a reputable medical physics journal serving both regional and global audiences.
MJ: What is your vision for SCMPCR, and where should the organisation focus its efforts in the coming years?
JJ: My vision is for SCMPCR to evolve into a leading regional centre for education, training, and research in medical physics and cancer care. The organisation should continue to prioritise capacity building in South Asia by delivering high-quality training programmes, workshops, and mentorship opportunities, particularly for early-career professionals.
Moving forward, SCMPCR should focus on standardising education and training across the region, promoting collaborative research, and strengthening clinical practice through quality assurance and patient safety initiatives. Increased attention should also be given to emerging areas such as artificial intelligence, advanced radiotherapy techniques, and modern imaging technologies.
Enhancing SCMPCR’s digital presence through online learning platforms and publications, including the proposed medical physics journal, will be vital. By strengthening partnerships with universities, hospitals, and international organisations, SCMPCR can play a transformative role in shaping the future of medical physics in South Asia and improving healthcare outcomes for patients.
MJ: This conversation with Dr. Jeyasingam Jeyasugiththan offers a compelling reflection on the evolving role of medical physicists in South Asia and the power of sustained regional collaboration. His professional journey spanning clinical service, academic leadership, research excellence, and capacity building, epitomises the spirit of commitment and resilience that SCMPCR seeks to nurture. Dr. Jeyasingam’s insights highlight not only the remarkable progress achieved in medical physics across the region but also the challenges that continue to demand collective effort, innovation, and vision. His contributions to the establishment of SCMPCR initiatives, particularly the SCMPCR Newsletter, underscore the importance of platforms that amplify professional voices, encourage mentorship, and foster a culture of shared learning. As SCMPCR moves forward, his perspectives reaffirm the need to strengthen education and training, embrace emerging technologies such as artificial intelligence, and uphold the highest standards of patient safety and quality assurance. Most importantly, this dialogue serves as an inspiration to young medical physicists, reminding us that meaningful progress is built through collaboration, ethical practice, and an unwavering focus on improving patient care.
On behalf of SCMPCR, I extend my sincere appreciation to Dr. Jeyasingam Jeyasugiththan for his enduring contributions and thoughtful reflections. His journey and vision continue to guide and inspire our collective efforts toward advancing medical physics and cancer care across South Asia.

Golam Abu Zakaria Receives Prestigious International Award
Asif Hasan Nabi
Alo Bhubon Trust, Dhaka, Bangladesh
The International Organization for Medical Physics (IOMP) has honoured Bangladeshi German scientist Professor Dr. Golam Abu Zakaria with the Harold Johns Medal for 2025, one of the highest international honours in the field of medical physics.

Professor Zakaria is a globally respected medical physicist who has made pioneering contributions in Radiation Oncology, Nuclear Medicine, and Diagnostic Radiology. In 2023, the German government recognized his outstanding service by awarding him the Federal Cross of Merit, its highest civilian honour.
A colleague first informed Professor Zakaria after seeing the announcement on the IOMP website. Shortly afterward, the IOMP President, Prof. Dr. John Damilakis officially contacted him to confirm the award. The medal was presented during the World Congress on Medical Physics and Biomedical Engineering (IUPESM 2025), held September 29 to October 4, 2025, in Adelaide, Australia. This congress occurs every three years.
This recognition highlights his decades of dedicated service to excellent teaching and contributions to international education and human development. Until his retirement six years ago, he headed the Department of Medical Physics at Gummersbach Academic Teaching Hospital, affiliated with the University of Cologne in Germany.
The German Society for Medical Physics (DGMP) congratulated him on its website, noting that this distinguished award recognizes his exceptional contributions in research, clinical innovation, and education. They emphasized his global impact, particularly through the creation of international training programs, academic development in Bangladesh, and long-term support for young professionals around the world.
Now 72, Professor Zakaria first travelled to Germany at the age of 18. Throughout his career, he has remained committed to supporting young medical physicists, especially those from developing countries in South Asia. He has facilitated numerous scholarships for students and medical physicists to pursue education and advanced training in Germany and established the DGMP Committee for Medical Physics in Developing Countries over three decades ago.
Though the Harold Johns Medal is a major honour, it adds to a long list of distinctions. He has previously been named “Outstanding Personality of the Decade 2000–2010” by two international oncology organizations. In 2019, Harvard Medical School awarded him the Global Radiation Oncology Distinguished Leader Award. The German government also recognized his work through the Federal Cross of Merit, acknowledging both his scientific achievements and his development work in Bangladesh.

Today, Professor Zakaria continues to supervise PhD students worldwide and is actively involved in developing the South Asia Centre for Medical Physics and Cancer Research (SCMPCR). Speaking to the media, he joked, “I had declined an earlier invitation to lecture in Adelaide because I did not feel like travelling so far. But now I really must go, because they are granting me a valuable award!” The Australian award marks a significant milestone in his life’s work.
Life and Work of Dr. Golam Abu Zakaria
Dr. Zakaria was born in Naogaon, Bangladesh, on December 31, 1953. He interrupted his studies at the Bangladesh University of Engineering and Technology (BUET) to travel to Germany in 1972 with a government scholarship. Here he completed his degree in Physics at the Martin Luther University of Halle-Wittenberg in 1978, pursued postgraduate studies at the University of Göttingen, and earned his PhD with distinction from Heidelberg University, followed by residency training in Medical Physics.
His doctoral research introduced the Electron Pencil Beam treatment technique for head, neck, and lung cancers. This innovation was used for more than ten years at Heidelberg University Hospital before commercial treatment planning systems became available.
For over three decades, he served as Head of Medical Radiation Physics and Chief Medical Physicist at the Gummersbach Academic Teaching Hospital, University of Cologne improving radiotherapy planning, dosimetry, and quality assurance. Since 2003, he has also been a Professor of Clinical Engineering at the Anhalt University of Applied Sciences.
He has played a key role in advancing Medical Physics education in Bangladesh. In 2000, he helped launch the country’s first Master’s program at Gono University. Later, he founded the South Asian Centre for Medical Physics and Cancer Research (SCMPCR), which trains cancer care professionals from across South Asia and beyond. He is also the founder of the Alo Bhubon Trust (Alo-BT), dedicated to improving education, healthcare, and training opportunities in Bangladesh.
Professor Zakaria has held numerous international leadership positions, including:
- Chair, DGMP Working Group for Developing Countries
- Vice-Chair, IOMP Accreditation Committee
- Chair, IMPCB Accreditation Committee 2 (Radiation Physics)
- Trainer for the ICTP Medical Physics Training Program
He has authored more than 120 scientific publications, including research on Artificial Intelligence in radiotherapy.
AFOMP has also established a Leadership Award in his name to inspire the next generation of medical physicists.

Athiyaman Mayilvaganan awarded with prestigious AMPI Meritorious Medical Physicist Award
Dr. Athiyaman Mayilvaganan, Associate Professor (Medical Physicist & Radiological Safety Officer) at Acharya Tulsi Regional Cancer Treatment & Research Institute, Sardar Patel Medical College & Associated Group of Hospitals, Bikaner, India was honoured with the prestigious AMPI Meritorious Medical Physicist Award at the national conference AMPICON 2025 in recognition of outstanding professional contributions to medical physics and cancer care.

Serving the institution since 2009, Dr. Athiyaman has played a transformative role in strengthening radiation oncology services across Western Rajasthan through key involvement in establishing the Tertiary Care Cancer Centre and commissioning advanced treatment technologies including the Bhabhatron-II Telecobalt Unit (2013), HDR Brachytherapy Unit (2016), Imaging System (2019), the TrueBeam Linear Accelerator (2020) — the first modern linear accelerator in any Government medical institution in Rajasthan — and the CT Simulator (2020).
Alongside clinical responsibilities, Dr. Athiyaman actively contributes to academics by training MD Radiation Oncology postgraduates, Radiological Technology students, and Medical Physics interns, and was instrumental in launching the Bachelor in Radiation Technology program. Under continued guidance, the institute remains the only Government medical institution in Rajasthan to run a continuous M.Sc. Medical Physics internship program with stipend support since 2017. Dr. Athiyaman is also an approved Ph.D. guide under Rajasthan University of Health Sciences, contributing to research growth and academic excellence in the field.

Hasin Anupama Azhari Elected President of AFOMP
South Asia Center for Medical Physics and Cancer Research (SCMPCR) is proud to announce that Prof. Dr. Hasin Anupama Azhari has been elected as the President of the Asia-Oceania Federation of Organizations for Medical Physics (AFOMP). This prestigious appointment marks a significant milestone for the medical physics community in Bangladesh and the Asia-Oceania region.

Prof. Dr. Hasin Anupama Azhari has long been a driving force in advancing medical physics nationally and internationally. She previously served as Vice President and Secretary General of AFOMP, where her leadership and vision greatly contributed to strengthening collaboration and professional development across member countries.
As the Secretary General of SCMPCR, Prof. Dr. Hasin Anupama Azhari has made remarkable contributions to the establishment and growth of medical physics education and training in Bangladesh and beyond. Her tireless efforts were instrumental in developing unified recruitment rules for medical physicists and in the creation of official medical physicist positions within the healthcare system.
Her election as AFOMP President is not only a recognition of her exceptional contributions but also an inspiration for all South Asian medical physicists. SCMCR extends its heartfelt congratulations and best wishes to Prof. Anupama for continued success in her new leadership role.


Celebrating IDMP 2025: BMPS Webinar Featuring Jin Xiance on AI Guided Radiotherapy
On November 7th, 2025, the Bangladesh Medical Physics Society (BMPS) organized a webinar to celebrate the International Day of Medical Physics (IDMP) 2025 under the global theme “Medical Physis and Emerging Technologies: Shaping the Next Decades”.

The event featured an expert lecture by Prof. Xiance Jin, Chief Medical Physicist, First Affiliated Hospital, Wenzhou Medical University, China. He delivered a highly informative talk on “AI Guided Radiotherapy”.
The session was moderated by Md. Jobairul Islam, Medical Physicist at Labaid Cancer Hospital and Superspecial Center, Dhaka, Bangladesh and Secretary of BMPS. The webinar provided an excellent platform for medical physicists, researchers, and students to enhance their understanding of the application of artificial Intelligence (AI) in Radiation Therapy.
Participants actively engaged in the discussion, appreciating the depth of insights shared by Prof. Jin. The session was well-received by the medical physics community and reflected BMPS’s continued commitment to professional development and knowledge exchange in the field of medical physics.

A new Era in Cancer Care: Bangladesh Commences Treatment with its first Tomotherapy System
Md. Fajle Rabby
Medical Physicist, TMSS Cancer Center, Bangladesh
On August 8, 2025, the TMSS Cancer Center in Bogura, Bangladesh, achieved a significant milestone in cancer care by inaugurating its Tomotherapy RADIXACT System. This event coincided with the TCC Cancer Congress 2025, a premier oncology conference held at the Momo Inn Hotel in Bogura. The dual-purpose ceremony underscored TMSS’s commitment to advancing cancer treatment and fostering knowledge exchange in the field of oncology.

The inauguration ceremony commenced with the unveiling of the first Tomotherapy RADIXACT System in Bangladesh. Following the inauguration, the TCC Cancer Congress 2025 brought together oncologists, radiologists, medical physicists, and researchers to discuss the latest advancements in cancer treatment and research. The Tomotherapy RADIXACT System capable of precision targeting which utilizes advanced imaging techniques to accurately locate and treat tumors. Adaptive Treatment is also possible by adjusting treatment plans in real-time to accommodate tumor movement and changes in patient anatomy. It is also capable of treating a wide range of cancers, including complex, pediatric cases and total body irradiation (TBI).
In the TCC Cancer Congress 2025, several keynote speeches are delivered by renowned experts in oncology and other fields related to oncology focusing on innovations in cancer treatment and research. Dr. M.A. Salam, Professor of Urology, Dr. Parvin Akhter Banu, Sr. Consultant of Oncology, Dr. Arman Reza Chowdhury, Senior Consultant of Radiation Oncology, Dr Habibullah Talukdar Raskin, Professor of Cancer Epidemiology and Preventive Oncology delivered their valuable speeches on different topics. Beside these, panel discussions were held on various topics such as precision medicine, radiotherapy advancements, and cancer prevention strategies. The congress served as a platform for knowledge exchange and collaboration among healthcare professionals, aiming to enhance cancer care standards in Bangladesh.
The inaugural ceremony was honored by the presence of Professor Dr. Omar Faruque Yusuf, the Vice Chancellor of Chattogram Medical University and Prof. Dr. Md. Abul Kalam Azad, Pro Vice-Chancellor (Administration), Bangladesh Medical University. It was also witnessed the presence of several distinguished dignitaries who added grandeur to the event. Prof. Dr. Moudud Hossain Alamgir, Executive Consultant, TMSS Health Sector; Rtn. Dr. Md. Matiur Rahman, Deputy Executive Director, TMSS; Mr. TM Ali Haider, Managing Director, Building Construction Limited; Prof. Dr. Md. Zakir Hossain, Principal, TMSS Medical College; Prof. Dr. AKM Ahsan Habib, Director, TMSS Cancer Center; and Md. Motiur Rahman (Mithu), Chief Medical Physicist and Assistant Project Director, TMSS Cancer Center, attended the program.

The inauguration of the Tomotherapy RADIXACT System, coupled with the TCC Cancer Congress 2025, marks a significant step forward in cancer care in Bangladesh. This event highlights TMSS’s dedication to providing cutting-edge treatment options and fostering a collaborative environment for medical professionals to share knowledge and expertise. With the support of esteemed leaders, TMSS continues to pave the way for innovative treatments and collaborative efforts in the fight against cancer.

BMPS President appointed as AFOMP Education & Training Committee Chair
It is a matter of great pride and pleasure for the Bangladesh Medical Physics Society (BMPS) to announce that Dr. Md. Akhtaruzzaman has been appointed as the Chair of the Education and Training Committee of the Asia-Oceania Federation of Organizations for Medical Physics (AFOMP).

This prestigious appointment reflects his longstanding contributions and leadership in the field of medical physics, both nationally and internationally. Dr. Akhtaruzzaman has been serving BMPS since its inception in 2009, holding various key executive positions over the years, and currently serves as the President of BMPS. Under his leadership, BMPS has expanded its academic and professional activities, fostering collaboration, capacity building, and educational advancements in medical physics across Bangladesh. Within AFOMP, Dr. Akhtaruzzaman has made significant contributions as a member of the Science Committee, Education and Training Committee, and Publication Committee.
His new role as Chair of the Education and Training Committee further recognizes his dedication to advancing professional standards and promoting high-quality education and training programs for medical physicists across the Asia-Oceania region. BMPS congratulates Dr. Md. Akhtaruzzaman on this remarkable achievement and wishes him continued success in his efforts to strengthen medical physics education, research, and professional development globally.

Medical Physics Day 2025 at AECH (NORI), Islamabad, Pakistan
Islamabad, Pakistan-November 22, 2025: Energy Commission Hospital (AECH), NORI Islamabad hosted Medical Physics Day 2025 with a full-day program that combined opening remarks, two technical sessions, poster session and Q&A segment.

The event opened with registration, followed by a formal inaugural session that included Holy recitation, the National Anthem, and welcome remarks. The session also highlighted the importance of the International Day of Medical Physics. Attention was drawn to the vital role medical physicist’s play in modern healthcare. Emphasis was placed on patient safety, quality assurance, and the growing responsibility of the profession in advancing clinical practice.
First Technical Session: Clinical Practice, Safety, and Advanced Planning
The first technical session focused on strengthening clinical practice and supporting the growth of medical physics in Pakistan through quality, safety, training, and research. Topics included “Introduction to POMP, where do we stand” and “Strengthening Clinical Practice through Implementation of Peer Review Practice in Medical Physics.”
The session also covered patient protection and internal dosimetry, along with technology and treatment-planning themes. Presentations discussed internal dosimetry and patient protection, innovations in isotope production, and treatment techniques such as SFRT using grid. Research oriented talks highlighted precision methods and computational tools, including personalized internal dosimetry of [¹⁷⁷Lu] Lu-hydroxyapatite for radiosynovectomy, efficiency analysis of spine SBRT across platforms, and a Python-integrated TOPAS framework for compensator design and variable RBE analysis in proton beam therapy.
A dedicated Q&A and poster display followed, allowing participants to engage directly with the presented work before the lunch break.
Second Technical Session: Measurement, Emerging Modalities, and Future Directions
The second technical session highlighted practical measurement workflows, advanced modalities, and future-facing tools for clinical and research use. It included work on CyberKnife beam characterization, such as measurement of off-center ratios (OCRs) using Gafchromic EBT3 films for variable apertures.
Emerging and advanced treatment approaches were also discussed, including accelerator-driven BNCT for cancer care and Monte Carlo–based investigations such as Geant4 dosimetric analysis for radiotherapy in patients with specific implants.
The session further explored digital transformation in the field through Generative AI-based medical physics reference applications, and it addressed the future trend of dosimetry audits in Pakistan, emphasizing the role of independent verification and continuous improvement in patient safety.
Community Impact and Closing

Programs like this strengthen the medical physics community. They create a shared space for learning. They also help connect clinical needs with research ideas. When medical physicists discuss peer review, dosimetry, advanced planning, and audits together, the whole system becomes safer and more consistent.
The event concluded with participant comments, concluding remarks, and a formal summary and appreciation for attendees and contributors.

The KYAMCH Cancer Center Marks International Day of Medical Physics (IDMP) – 2025 by Emphasizing the Emerging Technology
Parvez Mosharaf1, Md. Imrul Kaes2
1Dept. of Oncology & 2Dept. of Pediatric Haematology & Oncology
KYAMCH Cancer Center, Enayetpur, Sirajganj, Bangladesh
On November 07, the Medical Physics Division of Khwaja Yunus Ali Medical College & Hospital (KYAMCH) Cancer Center proudly celebrated the International Day of Medical Physics (IDMP) 2025. The event took place at the Dr. M. M. Amjad Hussain auditorium, where a full day of academic discussion revolved around the global theme: “Medical Physics and Emerging Technologies: Shaping the Next Decade”.

The gathering showcased esteemed speakers, including a virtual keynote from Prof. Dr. Golam Abu Zakaria, a trailblazer in medical physics education in Bangladesh. He accentuated “New Aspects of Medical Physics in radiation Oncology and Imaging” and also emphasized the importance of qualified Medical Physicist to ensure accuracy & safety in healthcare. Alongside, the event was graced by in-person presence of Prof. Dr. Hasin Anupama Azhari, President of the Asia-Oceania Federation of Organizations for Medical Physics (AFOMP). She highlighted “Structure, Aims and Functions of AFOMP”. Both speakers also underscored the urgent necessity for enhanced academic training and adherence to international standard in radiotherapy.
Conversations during the event illuminated the changing landscape of medical physicist’s role within multidisciplinary cancer care. The program culminated in a ceremony that celebrated excellence in radiotherapy treatment, reinforcing KYAMCH’s dedication to clinical precision. The session featured by Md. Yusuf, Honorable Society Director of KYAMCH, as the chief guest. He advised “Work together and be a hope for cancer patient” and also gave his heartfelt appreciation to all medical physicist’s whose work silently powers the precision and progress of modern medicine.
Founded in 2007, by visionary legendary Dr. Mir Mohammad Amjad Hussain, the KYAMCH Cancer Center proudly upholds its reputation as a frontrunner in regional oncology, having pioneered the first LINAC services beyond the capital city. KYAMCH Cancer Center believe that oncologists, medical physicists, technologists, nurses together is a team, all of their dedication and compassion ensure world-class cancer treatment even in a resource-constrained environment.


Solve it!!

SCMPR Newsletter is carry a new column – SOLVE IT! – featuring a relatively difficult question / interesting problem for the young medical physics students and young medical physicists to solve. Those who are interested can send their answers to sptgnadar@gmail.com . The best answer would get published in the next issue of the Newsletter along with the name and affiliation of the contributor.
In a conventional C-arm linac which has a maximum field size of 40 cm x 40 cm, the corners of fields larger than a certain size are clipped. See the picture below of a 40 cm x 40 cm field. The corners of the field are clipped

Questions:
1) Which is/are the component(s) in the linac head responsible for the clipping of the radiation field corners?
2) What is the largest possible square field size that can be obtained without its corners clipped? Explain your answer using the linac head geometry.

Solution: Problem (July 2025/ Volume 7/ Issue 2

1. A patient has to be treated by a direct 6 MV posterior spinal field of size 6 cm (width) x 48 cm (length) at an extended SSD of 120 cm. The prescribed dose is 1.8 Gy at a depth of 5.5 cm.
Data (output at dmax for 100 cm SSD, TMR) are given in the tables below. Using ONLY the data given in the tables, find out the treatment MUs.
Note: For equivalent square field, use the formula: Side of the square = 4*(area/perimeter)
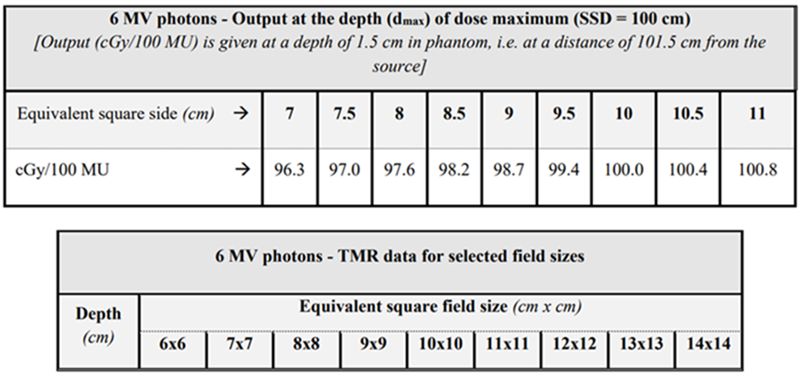
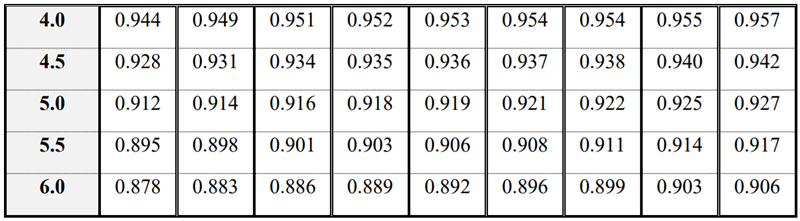
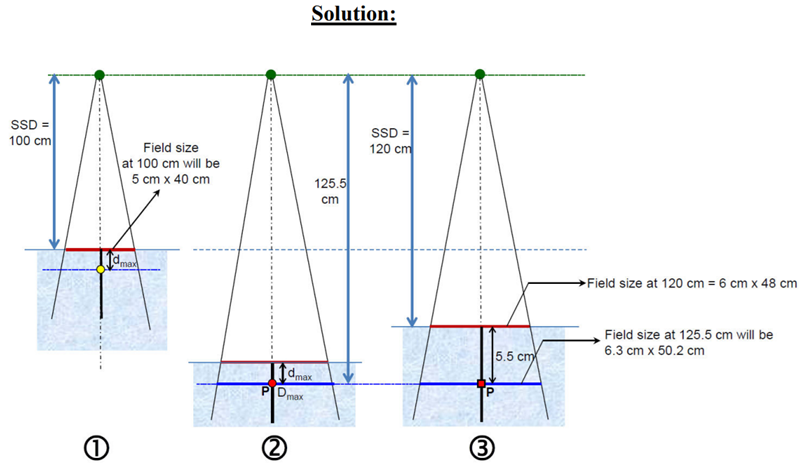
Please see Figs 1, 2 and 3
Field size at the extended SSD 120 cm = 6 cm x 48 cm
Field size at the treatment depth of 5.5 cm (i.e. at 125.5 cm from source) = 6.3 cm x 50.2 cm
Field size at the nominal SSD 100 cm = 5 cm x 40 cm
To use TMR data, the relevant geometry is Fig 2 and 3. The ratio of dose at the treatment depth of 5.5 cm to the dose at the same point with only dmax thickness of overlying tissue (i.e., the dose at red square in Fig 3 to the dose at the red circle in Fig 2) is the TMR for the field size of 6.3 cm x 50.2 cm. The equivalent square is 11.2 cm x 11.2 cm. The TMR (11.2 cm, 5.5 cm) = 0.9086.
To know the output at point P (the red circle) in Fig 2, we need to know the output at the dmax depth (yellow circle) in Fig 1.
Output for the field size of 5 cm x 40 cm (eq. sq = 8.9 cm) at 100 cm SSD = 98.6 cGy/100 MUs
Applying inverse square law, 98.6 cGy/100 MU * (101.52/125.52) 64.5 cGy/100 MUs at P (red circle)
The dose rate at the treatment depth (red square in Fig 3) = 64.5 cGy/100 MUs * 0.9086
= 58.6 cGy/100 MUs
To deliver a dose 180 cGy the required MUs = 100 MU/58.6 cGy * 180 cGy = 307 MUs

SCMPCR Newsletter Submission Guidelines
The following guidelines are provided to ensure consistency, clarity, and smooth compilation of the Newsletter.
All contributors are requested to follow these requirements strictly.
1. Overall Length
- Maximum total pages of the newsletter: 30 pages
2. Types of Submissions & Page Limits
A. SCMPCR Report
- Maximum length: 3 pages
- Maximum number of photographs: 4
- Photos must be submitted separately (not embedded in the document), each with a clear caption.
B. General Articles
- Total allocation: 3–4 pages
- May include maximum two general articles depending on length.
- Photos, tables, graphs must be sent as separate files with proper captions.
- Must follow APA reference style
C. Scientific Articles
- Maximum: 5000 words per article
- May include maximum two scientific articles depending on length.
- Photos, tables, graphs must be sent as separate files with proper captions.
- Must follow APA reference style
D. News & Events
- Maximum length: 1 page
- Maximum photos: 1 photo with caption (to be submitted separately)
- Should focus on recent, relevant activities or announcements
E. Awards & Honors
- Maximum length: ½ page
- Must include a photo of the awardee(s) submitted separately
- Include award title, date, venue, and a concise description (50–100 words)
3. Formatting Requirements
- Font: Times New Roman
- Size: 11 pt
- Line spacing: Single
- Submit in Word format (.doc or .docx)
- Do not apply any special formatting, columns, or layout—the designer will format accordingly.
Tables, Figures & Photos
- Must be submitted separately as image files (JPEG/PNG/TIFF preferred)
- Do not embed inside Word files
- Each table/figure/photo must have:
- Caption
- Numbering (e.g., Figure 1, Table 1)
4. Referencing
- All references must follow APA Style (7th Edition).
- Ensure accuracy and completeness before submission.
5. Authorship and Submission Ethics
- Write-up must not be generated by AI.
- AI may only be used for language editing, proofreading, or grammar correction.
- Authors are responsible for ensuring:
- Originality of the content
- Accuracy of data and references
- Proper permission for any photos used
6. Submission Checklist
Before submitting, ensure:
- Word file in 11 pt Times New Roman
- No embedded photos or tables
- All images/tables sent separately with captions
- Word count and page limits followed
- APA references checked
- AI-generated content not used for writing the article
- Author name, designation, affiliation, and email provided

